Human embryonic stem cells (ES cells) have, for the first time, been used to grow a crucial part of the eye, a paper in Cell Stem Cell reports. It is hoped that in the future transplantation of such tissue could help visually impaired people recover their sight.
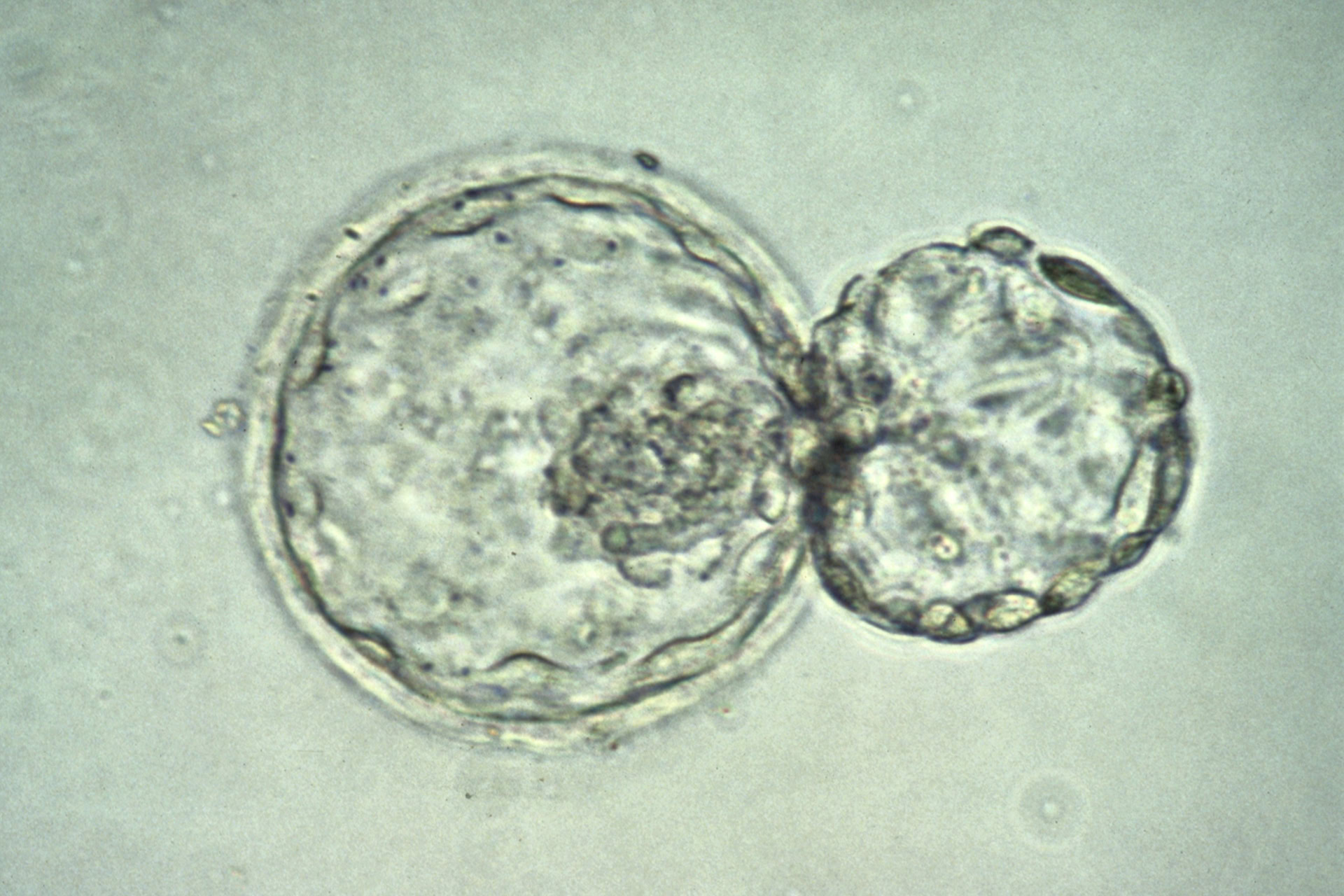
Scientists working at the RIKEN Centre for Developmental Biology in Kobe, Japan, managed to encourage human ES cells to self-organise into a three-dimensional and multi-layered human eye precursors, called an optic cup. The cup, just over half a millimetre in diameter, contained the important light-sensitive rod and cone cells - called photoreceptors - on its inner surface, as well as retinal cells in its outer wall.
As Professor Austin Smith, director of the Centre for Stem Cell Research in Cambridge, UK, who was not involved in the study, told Nature: 'The morphology [of the optic cup] is a truly extraordinary thing'. But only very recently have researchers been able to grow stem cells in three dimensions rather than as two-dimensional sheets in a dish. The optic cup self-assembled into its complicated three-dimensional shape without any direction, morphologically speaking, from the scientists.
Similar experiments done with mouse ES cells result in an optic cup that is much smaller - about one tenth the volume of that achieved with human ES cells. This suggests that final size of a tissue might be governed by innate characteristics of the cells themselves rather than by factors such as how much space a tissue has to grow into. Speaking to Nature, Professor Martin Pera, a stem cell biologist at the University of Southern California, said: 'The fact that size is cell-intrinsic is tremendously interesting'.
This research could pave the way for optic cups grown in the lab to be transplanted into human eyes as treatment for visual impairment. Importantly, the optic cup seems to be free of residual stem cells which, if left, could cause cancer or the growth of other cell types after transplantation. However, there are still major hurdles to be overcome and any treatment that uses the technology could be decades away. In the first instance, Professor Smith told Nature, the work needed to be independently assessed: 'We need to know how robust, how reproducible it is'.
In related news, a separate team of Japanese scientists announced they had coaxed human iPS cells, induced pluripotent stem cells, to form into a functioning human liver bud.
Although only five millimetres in size, the liver bud was able to break down drug compounds and express many human liver proteins. The liver also contained functional blood vessels though it lacked bile ducts and did not form as precisely organised a structure as natural livers.
Professor Stuart Forbes, a liver regeneration expert at the University of Edinburgh told Nature that the work 'sounds like a genuine advance'. Though scientists are some way off being able to grow full-size human livers, these new rudimentary livers could be used immediately for toxicity testing of drugs.
The work was presented at the International Society for Stem Cell Research conference by Dr Takanori Takebe of Yokohama City University, but is not yet published. According to Nature, session chair Professor George Daley from Boston Children's Hospital in the USA said, the research 'blew my mind'.
Sources and References
-
Rudimentary liver grown in vitro
-
Tiny human liver grown inside mouse's head
-
Japan team create liver from stem cells: report
-
Primitive Eye, Tiny Liver Grown in the Lab
-
Self-Formation of Optic Cups and Storable Stratified Neural Retina from Human ESCs
-
Biologists grow human-eye precursor from stem cells
-
Scientists see new hope for restoring vision with stem cell help
-
Blindness breakthrough as scientists turn stem cells into tissue that allows humans to see





Leave a Reply
You must be logged in to post a comment.